The tibial plateau fracture represents one of the most challenging orthopedic injuries affecting the knee joint. This complex injury involves a break in the upper portion of the tibia, specifically affecting the flat surfaces that form the foundation of the knee joint. Understanding the causes, diagnosis, and treatment options for this serious injury is crucial for both healthcare professionals and patients facing this condition.
Understanding the Tibial Plateau
The tibial plateau consists of two distinct areas: the medial (inner) and lateral (outer) plateaus. These smooth, relatively flat surfaces provide the foundation upon which the femur rests, creating the knee joint’s primary weight-bearing surfaces. The tibial plateau is covered with articular cartilage and supported by meniscal tissues, making it essential for proper knee function and stability.
When a tibial plateau fracture occurs, it disrupts this critical anatomical structure, potentially affecting joint alignment, stability, and long-term function. The injury can range from simple, non-displaced fractures to complex, multi-fragmentary breaks that require extensive surgical intervention.
Common Causes of Tibial Plateau Fractures
Several mechanisms can lead to a tibial plateau fracture, with the specific cause often determining the fracture pattern and severity. High-energy trauma represents the most common cause, particularly motor vehicle accidents where the knee strikes the dashboard or undergoes severe twisting forces. These incidents typically result in complex fracture patterns that may involve both plateaus and surrounding soft tissues.
Sports-related injuries constitute another significant cause, especially in activities involving pivoting, jumping, or contact. Skiing accidents, football injuries, and cycling crashes frequently result in tibial plateau fractures due to the rotational and compressive forces applied to the knee during these activities.
Falls from significant heights can also cause this injury, particularly when an individual lands on their feet with the knee in a vulnerable position. The axial loading forces transmitted through the femur to the tibial plateau can exceed the bone’s structural limits, resulting in fracture.
In older adults, particularly those with osteoporosis, even relatively minor trauma can cause a tibial plateau fracture. Age-related bone density loss makes the tibial plateau more susceptible to fracture from falls or minor accidents that might not injure younger individuals.
Classification and Types
Medical professionals classify tibial plateau fractures using several systems, with the Schatzker classification being the most widely used. This system categorizes fractures into six types based on fracture pattern and location:
Type I fractures involve a lateral plateau split without depression, typically seen in younger patients with strong bone quality. Type II fractures combine a lateral split with depression of the articular surface. Type III fractures present as pure lateral plateau depression, commonly occurring in older patients with osteoporotic bone.
Type IV fractures affect the medial plateau, often associated with higher energy trauma and potential vascular injury. Type V fractures involve both plateaus in a bicondylar pattern, while Type VI fractures include plateau fractures with metaphyseal-diaphyseal dissociation, representing the most severe injury pattern.
Diagnostic Approaches
Accurate diagnosis of a tibial plateau fracture requires comprehensive clinical evaluation and advanced imaging. Initial assessment includes physical examination to evaluate knee stability, range of motion, and neurovascular status. However, imaging studies provide the definitive diagnosis and treatment planning information.
Plain radiographs serve as the initial imaging modality, providing basic fracture pattern information. However, computed tomography (CT) scans offer superior detail regarding fracture displacement, articular surface depression, and bone fragment location. Three-dimensional CT reconstruction helps surgeons better understand complex fracture patterns and plan appropriate treatment approaches.
Magnetic resonance imaging (MRI) may be utilized to evaluate associated soft tissue injuries, including meniscal tears, ligament damage, and cartilage injury, which commonly accompany tibial plateau fractures.
Non-Surgical Treatment Options
Not all tibial plateau fractures require surgical intervention. Non-displaced or minimally displaced fractures with maintained joint alignment may be suitable for conservative management. This approach typically involves initial immobilization using a knee brace or cast, followed by graduated weight-bearing restrictions.
The conservative treatment protocol usually begins with several weeks of non-weight-bearing status, allowing initial fracture healing. Physical therapy plays a crucial role in maintaining joint mobility and preventing stiffness during the immobilization period. Range of motion exercises typically begin early, while weight-bearing progression follows a carefully monitored schedule based on fracture healing progress.
Pain management during conservative treatment involves a multimodal approach, including anti-inflammatory medications, ice application, and elevation. Regular follow-up examinations with repeat imaging ensure proper fracture alignment maintenance throughout the healing process.
Surgical Treatment Approaches
Many tibial plateau fractures require surgical intervention to restore joint alignment, stability, and function. The surgical approach depends on fracture pattern, displacement degree, and patient factors such as age and activity level.
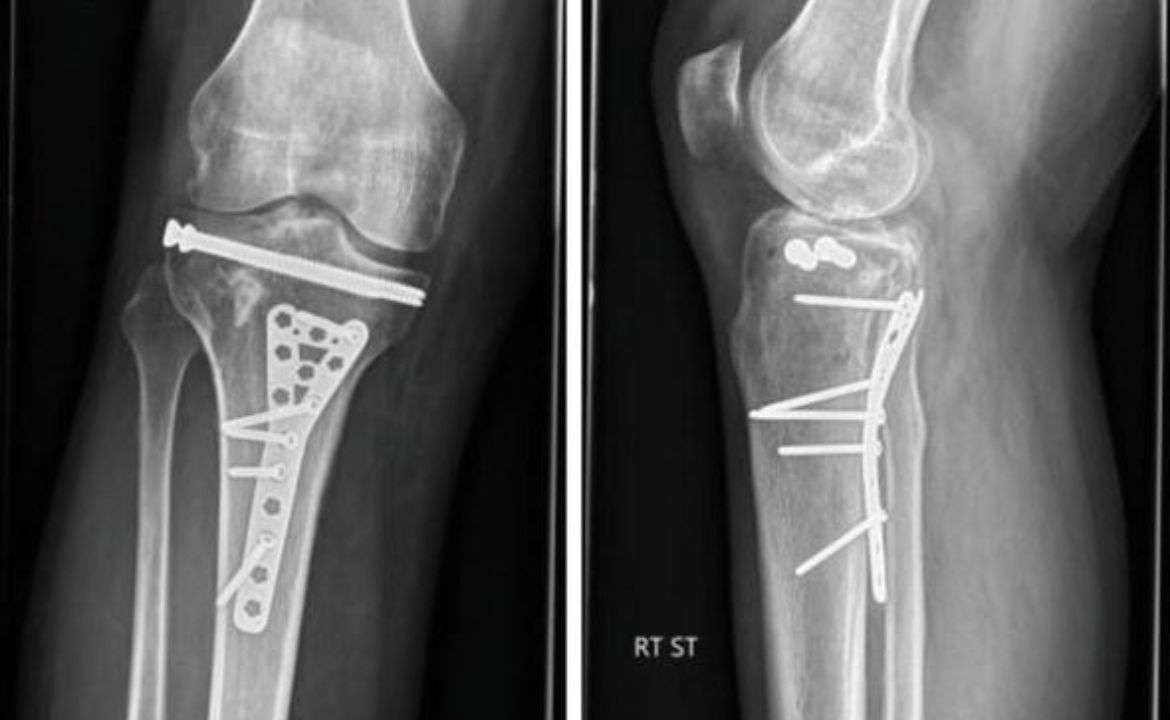
Open reduction and internal fixation (ORIF) represents the most common surgical approach for displaced fractures. This technique involves directly visualizing the fracture, reducing bone fragments to their anatomical position, and securing them with plates, screws, or other fixation devices. The surgical approach may be lateral, medial, or dual incision based on the fracture pattern.
For fractures with significant articular surface depression, bone grafting may be necessary to support the elevated joint surface and prevent collapse. Surgeons may use autograft bone from the patient’s iliac crest or synthetic bone graft substitutes to fill defects and provide structural support.
In severe cases with extensive soft tissue damage or compromised bone quality, external fixation may be employed as a temporizing measure or definitive treatment. This approach involves placing pins or wires through the bone above and below the fracture, connected to an external frame that maintains alignment and stability.
Recovery and Rehabilitation
Recovery from a tibial plateau fracture varies significantly based on fracture severity, treatment approach, and individual patient factors. The rehabilitation process typically extends several months and requires dedicated commitment to physical therapy and activity modification.
Initial recovery focuses on pain control, swelling reduction, and early range of motion exercises to prevent joint stiffness. Weight-bearing restrictions usually continue for 6-12 weeks, depending on fracture healing progress and surgical fixation stability.
Progressive physical therapy emphasizes quadriceps strengthening, knee flexion improvement, and functional movement pattern restoration. Advanced rehabilitation includes proprioceptive training, balance exercises, and sport-specific activities for appropriate candidates.
Long-term outcomes vary, with some patients experiencing excellent functional recovery while others may develop chronic pain, stiffness, or post-traumatic arthritis. Early recognition, appropriate treatment, and dedicated rehabilitation provide the best opportunity for optimal outcomes following this challenging injury.
Conclusion
The tibial plateau fracture represents a complex orthopedic injury requiring careful evaluation and individualized treatment planning. Understanding the various causes, from high-energy trauma to age-related fragility, helps in both prevention and early recognition. Whether managed conservatively or surgically, these injuries demand patience, dedication to rehabilitation, and realistic expectations regarding recovery timelines and outcomes. With appropriate treatment and commitment to the recovery process, many patients can achieve satisfactory functional outcomes and return to their desired activity levels.














Leave a Reply